Cary Ortho utilizes bone marrow stem cells for general orthopedic and spine treatment
Orthopedic stem cell treatment is the next frontier in treating orthopedic and spinal disorders. The Cary Orthopaedics team is leading the way.
Using stem cells harvested from an adult patient’s own bone marrow, Dr. Sameer Mathur and Dr. Nael Shanti – both board-certified orthopedic spinal surgeons – have developed a minimally invasive remedy for those suffering from degenerative disc disease, back pain and spinal arthritis.
Applying a similar approach, Cary Ortho’s physician assistant, Kevin G. Morrison, PA-C, a regenerative medicine specialist, uses stem cell therapy to give patients pain relief from osteoarthritis and soft tissue injuries.
Multiple research studies have shown a significant reduction in low back and joint pain and improved function after stem cell injections. While these treatments are still evolving, 80% to 90% of patients are reporting improvement in their symptoms after orthopedic stem cell treatments.
Conventional treatment for bone and joint degeneration
Many patients suffering from degenerative disc diseases or low back pain are often not ideal candidates for surgery. Some who have chosen to undergo surgery have had unsatisfactory results. Therefore, the typical remedy for chronic orthopedic conditions is extensive physical therapy combined with oral anti-inflammatory medications. The result: The majority of patients still have to live with pain.
Orthopedic and spine stem cell treatment
Bone marrow injections are a breakthrough for patients in pain. Cary Orthopaedics has been at the forefront of this technology. We incorporate bone marrow aspirate concentrate (BAC) into the treatment of both acute and chronic soft tissue and joint-related injuries.
Our physicians are utilizing orthopaedic stem cell treatment using the patient’s own bone marrow, the soft, spongy tissue found in the center of bones. Bone marrow in adults contains a rich reservoir of “multipotent” stem cells – also known as mesenchymal precursor cells (MPCs) – that can be extracted from the patient’s pelvis or hip bone.
Due to their unique, regenerative composition, these cells can become various types of tissues, including soft tissue, bone or cartilage. This makes them an excellent resource for repairing and rebuilding damaged tissue, accelerating the healing process and improving overall function.
Technological advancements have made the removal and harvesting process easier and less expensive. This minimally invasive procedure has fewer side effects than traditional surgery and causes minimal discomfort to the patient.
A growing body of research and results
Much of the previous research of stem cells had centered around placental stem cells, which can also adapt into other types of tissues. However, these have not performed well when put to the test for orthopaedic treatment. Bone marrow aspirate concentrate provides MPCs that can transform into osteocytes, chondrocytes and adipocytes, all of which are important in treating orthopedic conditions.
The latest research around mesenchymal stem cells, specifically bone marrow aspiration, is certainly promising. Cary Orthopaedics continues to collect data and review patients’ responses.
Bone marrow stem cells for degenerative disc disease and back pain
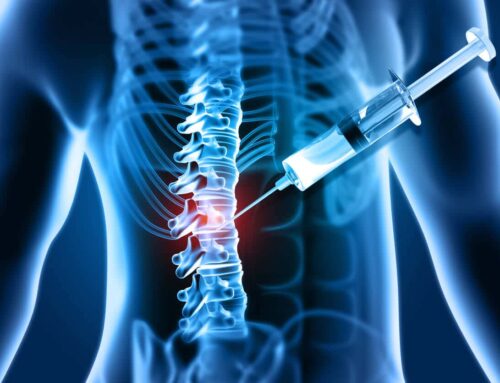
Dr. Mathur at Cary Ortho has performed stem cell spine injections for nearly a decade, treating degenerative disc disease of the lumbar spine. We harvest bone marrow from the patient’s pelvic bone and isolate the stem cells. We then inject the ultra-concentrated stem cells into the degenerative disc in the lower back.
“I’m very excited about our outcomes,” Mathur comments. “We have completed hundreds of stem cell injections, with an 80% to 90% success rate. It appears the stem cells are slowing the inflammatory cascade in the degenerative disc and helping people with back pain.”
Mathur continues: “Stem cells are a great option for patients, especially those 60 years of age or younger with low back pain. We are seeing two types of patients who come to us. The first group is patients with severe lower back pain who have been told they need fusion surgery. They want to avoid extensive surgery, and in some cases, stem cells can be the answer.
“The other growing group is younger patients that have degenerative discs and mild pain but want to prevent their disc from getting worse. Using stem cells to prevent future problems is the most exciting aspect for me. I love it when we can stop the degeneration at an early stage to prevent the need for surgery in the future.”
Dr. Mathur has been instrumental in elevating the patient care level at Cary Orthopaedic Spine Center since joining the practice in 2008. He attended medical school at the University of Pennsylvania and a spinal reconstructive fellowship at the Rush University Medical Center in Chicago. He also taught at Dana Farber Cancer Institute in Boston. Over the last 15 years, in conjunction with the National Institutes of Health, he has conducted significant studies of disc degeneration and analysis of the expression of genes that may damage the disc.
“In the past decade, there have been several advancements in spinal surgery, but regenerative medicine is the next frontier,” said Dr. Mathur. “I see so many patients that have low back pain and leg pain from degenerative disc disease. For many, there is no good surgical treatment option, and stem cell injections may be a viable option.”
As an orthopaedic spine specialist, Dr. Mathur is an expert in spinal surgery and the diagnosis and treatment of a wide range of spinal problems. His depth of experience allows him to determine whether a patient would benefit from physical therapy, stem cell injections or surgical intervention.
Cary Ortho’s Dr. Shanti is also well versed in stem cell treatment for spinal conditions. “There is currently extensive, ongoing research on the application of stem cell therapy and tissue regeneration, including an application for spinal cord injury and disc pathology, which is very exciting,” said Dr. Shanti.
Recognized as Top Orthopaedic Doctor by The Leading Physicians of the World for the outstanding patient care, Dr. Shanti’s in-depth experience and understanding of the spine allows him to guide his patients – especially those with chronic back pain – to the most appropriate path of treatment.
Dr. Shanti completed his spine surgery fellowship training at the prestigious New England Baptist Hospital, Tufts University program with an emphasis on minimally invasive spine surgery. He has authored and presented multiple papers and textbooks on the advancement of minimally invasive spine surgery.
Bone marrow stem cells for osteoarthritis and joint pain relief
According to regenerative medicine specialist and PA Kevin Morrison, stem cell therapy can also be used to treat other joints in the body, with relieving knee pain being a key focus.
“We’ve found that stem cell therapy can be very safe and effective when used with the appropriate patient population,” said Morrison. “Feedback has been quite positive, and we continue to watch long-term data.”
How the stem cell procedure works
The stem cell injection is a same-day procedure that generally takes about one hour. The actual extraction of bone marrow takes up to 10 minutes.
The bone marrow extraction site – typically the back of the patient’s hip or pelvis bone – is numbed using a mixture of local anesthetics. A suctioned syringe is attached to a long needle that reaches the posterior aspect of the hip. The patient may experience a minimal amount of discomfort during the extraction.
The sample is collected, transferred through a filter and then placed into a centrifuge for spinning. The speed separates the stem cells and platelets from the bone marrow. This concentration of stem cells is then reintroduced into the painful area under image guidance with fluoroscopy to confirm accurate placement.
The harvesting site will be numb for one to two hours after the procedure, so the patient will need transportation home. It is permissible to fly after the treatment, but this may cause increased pain or discomfort.
When administering stem cell treatment, Cary Ortho performs a single injection for all patients, whereas some clinics typically require multiple injections over several weeks.
Healing time
Orthopedic stem cell treatment relies on the body’s own regenerative process to heal, which takes time. Patients have seen the benefits in two to three months after treatment; however, many have noticed improvements in symptoms sooner.
Age requirements
The recommended age range for the treatment is 20 to 70. As the body ages, the quality and quantity of stem cells slowly decline. After age 70, patients may experience a sharper decline in stem cells, resulting in less beneficial outcomes.
Request a consultation for orthopedic stem cell therapy
Orthopaedic stem cell treatment is an excellent solution for patients with degenerative disc disease and those suffering from arthritis of the spine, bulging disc, low back pain, facet joint pain or disc with annular tears.
Stem cell treatment is appropriate for patients with very specific conditions and is not covered by most insurance carriers. The cost of the procedure can range from $5,000 to $7000.
If you think you might be a candidate for orthopedic stem cell therapy treatment, contact Cary Orthopaedics to schedule a consultation. Our regenerative medicine physicians will evaluate each patient individually to determine if they are a good candidate for stem cells.