WHAT OUR PATIENTS ARE SAYING
Dr. Martini was absolutely amazing. He was gentle and administering my shots and made sure I was comfortable. Dr. Martini genuinely cares for his patients. I would highly recommend Cary Orthopaedics.
Dr. Bullock is the most caring & knowledgeable physician I have ever met. She has passion! You are not just a number. I have been to over three different ortho groups in the last 55 years for broken bones & surgeries. Cary Ortho is lucky to have her.
Dr. Curzan is an absolutely amazing doctor. He has wonderful bedside manner. Greets you like an old friend and puts you at ease. He tries very hard to get to the root of your problem and does what he can to make you feel better. He has been my doctor for over four years, and I wouldn’t think of going to anyone else.
My first visit to see Dr. Mathur felt very comfortable, and his staff were all AAA. Great experience. His PA was also awesome, great bedside manner. Cary Ortho has a great team!
Service was surprisingly delightful and was a professional setting. The doctor provided an educational, entertaining, friendly, inviting and innovative experience. The team and everyone there was friendly. My condition feels better already. Would definitely recommend Dr. Reinke.
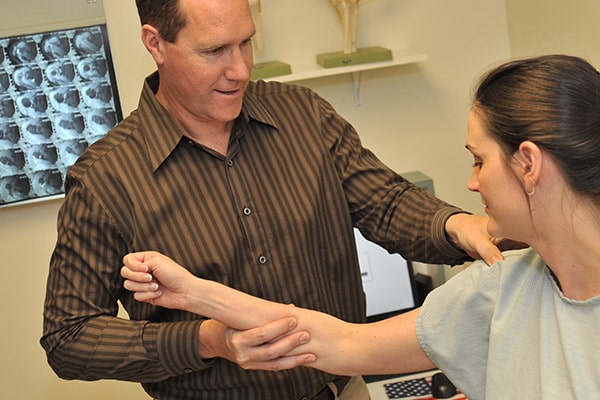
Sports Medicine
Professional and recreational athletes alike can succumb to injuries. At Cary Orthopaedics, our sports medicine specialists are dedicated to getting you back on the court, field, rink or pool as quickly and safely as possible.
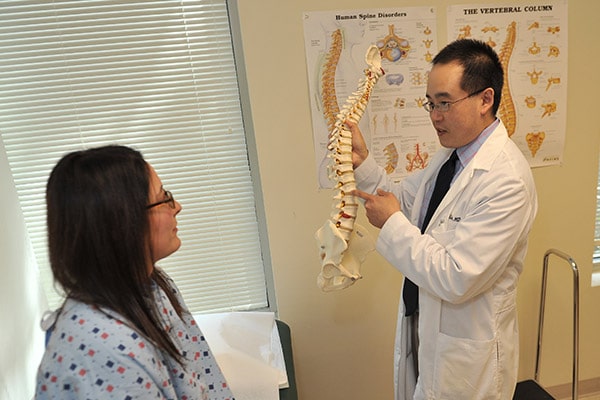
Spine Center
Maintaining a strong, healthy spine is critical to your overall wellness and longevity. Cary Orthopaedics has the region’s only comprehensive Spine Center offering a full range of spine care, including minimally invasive spine surgery.
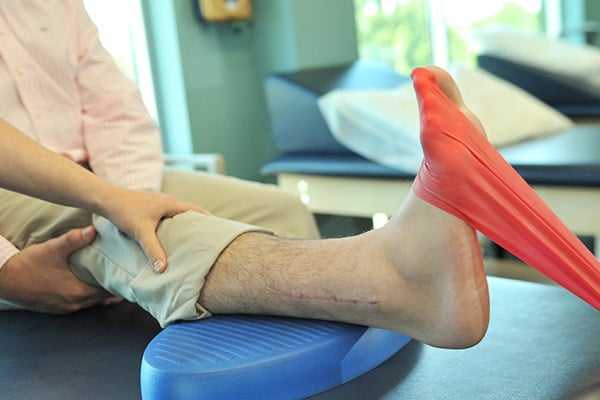
Physical Therapy
Individualized physical therapy addresses specific orthopaedic injuries and conditions. With a bio-mechanical and neuromuscular evaluation, we pinpoint the best treatment to relieve pain, prevent recurrence, and restore strength and mobility.
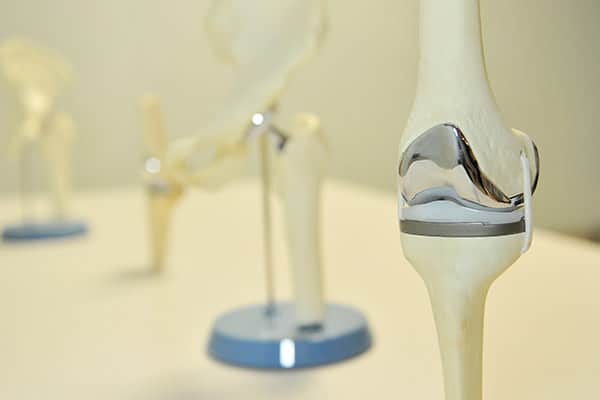
Joint Replacement
Cary Orthopaedics offers total joint replacement surgery to replace painful hip, knee and shoulder joints. Our experienced physicians perform hundreds of joint replacements each year.
Since 1982, Cary Orthopaedics has delivered excellence in orthopaedic care to address bone and joint pain or dysfunction caused by trauma, sports injuries and degenerative conditions.
Our board-certified orthopaedic doctors and orthopaedic care teams strive to bring good health and mobility to our patients.